Summary
Healthcare workers must be physically active, quick-witted, and emotionally resilient. These obligations are compounded by the additional difficulty of fasting from sunrise till sunset for nurses and nursing students who observe the holy month of Ramadan. Controlling your blood sugar levels is one of the most important factors of preserving your health and professional effectiveness throughout this period. Your body needs a constant supply of glucose to power your muscles and, more crucially, your brain over a 12-hour shift. Your capacity to determine drug dosages, track patient vital signs, and handle crises may be compromised if your blood sugar falls too low (hypoglycemia) or rises too high and then crashes (hyperglycemia) can be significantly impaired.
For nurses, controlling blood sugar is essential to patient safety and goes beyond personal comfort. With the correct nutritional approach, a “brain fog” brought on by falling glucose levels can result in clinical mistakes that are completely avoidable. The healthiest things to eat to maintain a “steady state” of glucose, how the human body uses energy during a fast, and how to spot the clinical warning signals that your blood sugar is approaching a dangerous level are all covered in detail in this article. You can achieve both professional success and spiritual fulfillment by treating your own metabolic health with the same care that you give your patients.
The Science of Glucose and Insulin During a Fast
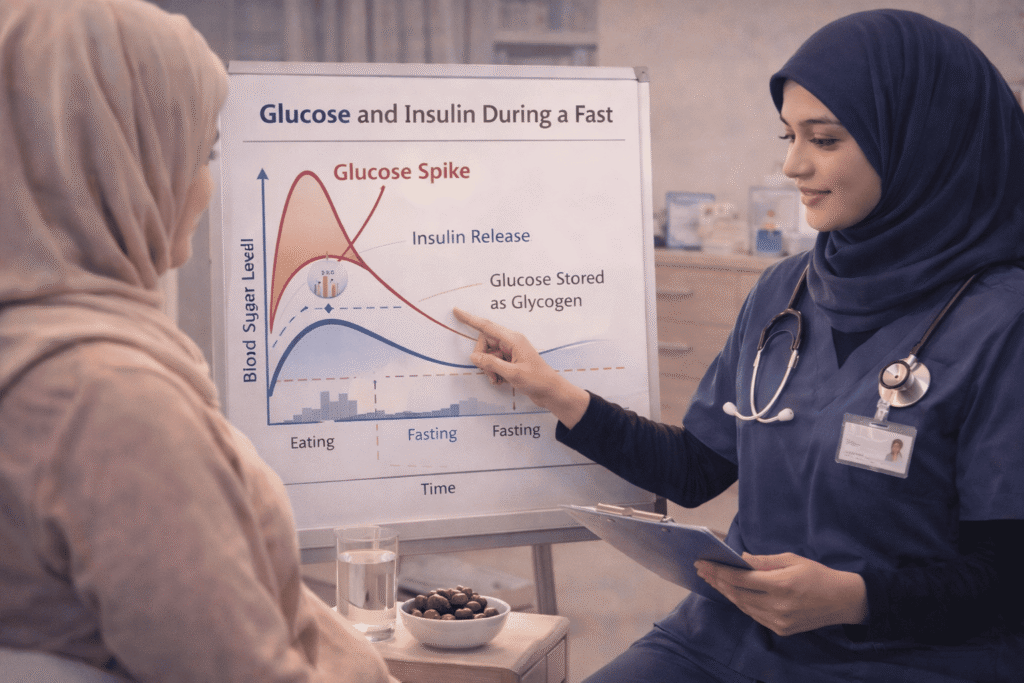
Understanding how your body fuels itself while you’re not eating is the first step towards efficiently managing your blood sugar. Normally, when we eat, our bodies convert carbs into glucose, which is then released into the blood. The hormone insulin, which functions as a key and allows glucose to enter our cells for use as fuel, is then released by the pancreas. During Ramadan, the body goes into a “fasting state” four to six hours after Suhoor, when the glucose from your last meal is depleted. In order to maintain stable levels, the liver now starts to release stored glucose, or glycogen.
This shift is critical for a nurse working on a busy ward. Eating high-sugar dishes at Suhoor causes a significant rise in insulin levels. By removing too much sugar from the blood, this insulin “overshoots” its function and causes a sudden fall. Because of this, you may feel full of energy at 8:00 AM but entirely worn out and unsteady by 11:00 AM. Knowing this cycle enables you to select foods that avoid these sharp “peaks and valleys.” You can make sure that your muscles and liver have a consistent supply of fuel until the sunset Iftar by concentrating on foods that call for a slow, steady release of insulin.
Strategic Suhoor: The Foundation of Glycemic Stability

Suhoor is the most crucial therapeutic intervention of the day for a fasting nurse. Your “fuel tank” for the next 14 to 16 hours is this meal. Low-Glycemic Index (GI) foods must be your top priority if you want to keep your blood sugar constant. These foods slow down the rate at which blood sugar rises and falls. Choosing “white” carbs, such as white bread, sugary cereals, or white rice, puts you at risk for an energy deficit in the middle of your shift.
The three primary ingredients of a “Nurse-Approved Suhoor” are Complex Carbs, Lean Protein, and Healthy Fats. Fiber from complex carbohydrates, such as whole-grain rye, barley, and steel-cut oats, slows down digestion. In addition to providing the amino acids required for muscle repair, protein from beans, Greek yogurt, or eggs keeps you feeling full. As a “buffer,” healthy fats like nuts, avocados, or olive oil further reduce the rate at which glucose enters the bloodstream. A “time-release” energy effect is produced by this combination. For instance, a plate of pancakes or sweet pastries is far less productive for a 12-hour shift than a bowl of oatmeal with walnuts on top and a side of hard-boiled eggs.
Recognizing Hypoglycemia on the Ward
The intense physical demands of breastfeeding can occasionally result in hypoglycemia, or low blood sugar, despite your best efforts during Suhoor. Although you are trained as a nurse to identify these symptoms in your patients, it is frequently more difficult to identify them in yourself when you are preoccupied with providing care. Shakiness, sweating, palpitations, and extreme hunger are some of the early signs. But cognitive symptoms confusion, impatience, and loss of focus are the most harmful for a medical practitioner.
Your blood sugar may be falling below the safe range if you begin to feel “spaced out” or find yourself reading a drug label several times because you are unable to concentrate. This is a “Red Flag” in a medical setting, thus you need to have a strategy in place. This entails taking a time to sit down and telling a coworker that you’re feeling under the weather. The safety of your patients is your top ethical duty, even while spiritual devotion is significant. If your hypoglycemia is severe, you need to break your fast with a quick-acting glucose source, such a date or a little drink, and then stabilize the level with a snack high in protein. Acknowledging your limitations is not a sign of spiritual weakness, but rather of professional development.
Iftar and the “Post-Prandial” Glucose Spike
The temptation is to have a big, high-calorie meal right away when the sun finally sets. However, a “heavy” Iftar can be detrimental for a nurse who needs to study after their shift or who could continue be on duty. Your blood sugar levels soar when you overindulge in high-sugar or high-fat foods while fasting. This results in a huge insulin release, which triggers a “rebound crash,” which leaves you feeling extremely drowsy and listless often referred to as a “food coma.”
The most effective approach is the “Two-Stage Iftar.” Water and two to three dates should be the first step, which should happen right away. Dates provide your blood sugar a controlled rise without the pandemonium of refined sugar because they are high in potassium and natural fiber. After a brief intermission (about 20 minutes), stage two should take place. This dish should resemble a nutritious supper: 50% of the plate should be made up of vegetables (fiber), 25% should be made up of lean protein (muscle repair), and 25% should be made up of complex grains. You can actually lessen the meal’s overall blood sugar surge by consuming your vegetables and protein before your carbs. If you need to return to the ward or complete your clinical record, this helps you stay focused.
Managing Blood Sugar for Night Shift Nurses
During Ramadan, nurses who perform night shifts have a particular difficulty. Their “fasting window” occurs while they are asleep, while their “eating window” occurs when they are working. These nurses’ circadian rhythm and blood sugar regulation are strongly related. At night, the body’s natural ability to metabolize glucose is diminished. This implies that a night shift nurse’s blood sugar will remain higher than it would during the day if they consume a big, sugary meal at 2:00 AM. This can result in inflammation and long-term health problems.
Throughout their shift, night shift nurses should concentrate on “Light and Frequent” fuelling. Eat smaller, high-protein snacks throughout the evening rather than a single, large meal during Iftar. As a result, blood sugar levels stay on a “level plane” as opposed to a roller coaster. Steer clear of the “midnight pizza” or vending machine food that are frequently available in hospital break rooms. Bring prepared food instead, such as apple slices with peanut butter, lentil soup, or chicken salad. Choose items that will help you fall asleep, such as a small bowl of fruit and yogurt, when it’s time for Suhoor at the conclusion of the night shift. You may safeguard your metabolic health and make sure you wake up feeling rejuvenated for your next shift by aligning your diet with your shift schedule.
People Also Ask (FAQ)
Q: Can I take my blood sugar with a finger-prick test while fasting?
Indeed. The majority of religious scholars and medical professionals concur that using a finger prick test to check your blood sugar levels does not violate your fast. In fact, it is strongly advised for nurses with pre-diabetes or diabetes to keep an eye on their blood sugar levels throughout extended shifts.
Q: Why do I get a headache in the afternoon while fasting?
It is frequently an indication of a drop in blood sugar or dehydration, though it can also represent caffeine withdrawal. Your blood sugar levels are too low if the headache is accompanied by lightheadedness or disorientation. Try to sleep in a cool place, and if it doesn’t go away, think about if you should break the fast for safety.
Q: Is it okay to use “glucose tabs” if I feel shaky on shift?
The purpose of glucose tablets is to rapidly elevate blood sugar. You are technically breaking your fast if you use one. However, you need to treat hypoglycemia right once if you are suffering symptoms while tending to patients. Patient safety and your clinical judgment are your top priorities.
Q: What is the best drink for staying hydrated and keeping sugar stable?
The most important thing is always water. Coconut water, on the other hand, is a great option for Iftar since it has natural electrolytes and a tiny bit of sugar that helps rehydrate your cells more efficiently than plain water without producing a significant sugar spike.
Q: How can I explain my need for a “glucose break” to my supervisor?
Take the initiative! Talk to your management briefly before Ramadan begins. “I’ll be fasting this month, and even though I intend to work my entire shift, I might need a 5-minute sit-down if I feel like my energy levels are dropping,” you could remark. I want to prioritize patient safety, but I have prepared for my Suhoor to remain steady.” The majority of supervisors will value your openness.
Useful Documents for every Nursing Student
CV Section Template for Nursing students
AHPRA – NMBA Registration Document Checklist (International Students-Graduates)
Clinical Placement Reflection Template (NMBA-aligned)
Cover Letter Template for Nursing Students
Disclaimer: “I researched this information on the internet; please use it as a guide and also reach out to a professional for assistance and advice.This information is not medical advice, so seek your medical professional’s assistance.”

