Summary
Providing care during Ramadan necessitates a careful balancing act between clinical knowledge, ethical sensitivity, and cultural humility for midwives and midwifery students. Due to the significant physiological changes that occur during pregnancy, a woman’s decision to fast complicates monitoring of both the mother and the fetus. Many pregnant women nevertheless opt to fast because of a strong spiritual connection to the month or a desire to take part in group worship, even though Islamic law clearly exempts them if they worry for their health or the health of their unborn child.
The midwife’s job is to offer a “safety net” of evidence-based advice, not to tell women whether or not to fast. You are the main teacher who explains to the mother how fasting impacts the chemistry of her body and the growth of her unborn child. You can make sure the mother feels empowered to make the greatest choice for her particular situation by providing nonjudgmental support. Midwives can use this article as a thorough guide to manage these consultations, keep an eye out for potential hazards, and offer dietary recommendations that put a good pregnancy result first.
The Physiology of Fasting in Pregnancy
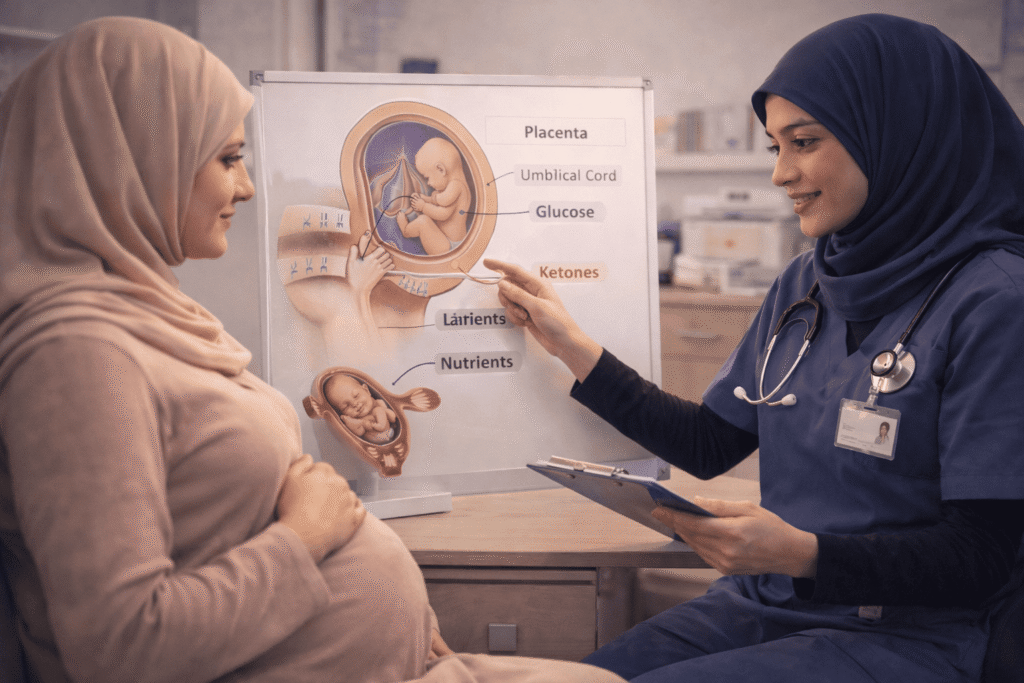
The first step in offering professional midwifery advice is to comprehend the physiologic changes that take place during a fast. The body of a pregnant woman experiences “accelerated starvation.” This implies that her blood glucose levels fall far more quickly when she quits eating than they would if she weren’t pregnant. Her body starts to break down fat reserves more quickly in order to make up for it, which causes ketones to be produced. High levels of ketones can penetrate the placenta and possibly impact fetal development, while lower amounts are normal.
Mothers must be informed by midwives that the infant needs a constant supply of nutrients and glucose through the umbilical chord. The infant is totally dependent on the mother’s internal resources when she fasts for 14 or 16 hours. The body is typically effective at this for a healthy lady with a normal BMI. However, this metabolic load might be serious for women who already have problems like gestational diabetes or anemia. In order to make sure that the “fasting gap” isn’t causing maternal fatigue or a reduction in fetal movement, midwives should keep a closer eye on fetal growth and maternal weight gain throughout this month.
Conducting a Clinical Risk Stratification

Since every pregnancy is unique, every woman’s “risk” of fasting varies. During their prenatal visits, midwives ought to employ a “Risk Stratification” strategy. This entails classifying women according to their present pregnant status and medical history. Compared to a healthy woman in her second trimester, a first-trimester woman experiencing Hyperemesis Gravidarum (severe morning sickness) is far more likely to experience electrolyte imbalance and dehydration.
In particular, midwives should search for “High-Risk” indicators such intrauterine growth restriction (IUGR), low amniotic fluid levels, or a history of premature labor. In these situations, the midwife is required to provide a detailed explanation of the health hazards associated with fasting. On the other hand, the midwife can offer a supporting framework for a “Low-Risk” woman, teaching her how to fast safely and stressing that the fast must be ended if specific symptoms manifest. By customizing the treatment plan, the midwife upholds the woman’s autonomy while carrying out her professional obligation to “Do No Harm.”
Monitoring Fetal Wellbeing and “Red Flags”
Teaching the mother how to keep an eye on her infant at home is a fundamental component of midwifery education during Ramadan. Fetal movement is the most significant measure of fetal health. Mothers should be instructed by midwives to complete “Kick Counts” throughout the day, particularly in the late afternoon when their blood sugar levels are at their lowest. The mother must break her fast right away and get in touch with the maternity hospital if she observes a noticeable decline in the baby’s movements.
The midwife is responsible for teaching the mother about fetal activity as well as “Maternal Red Flags.” These include intense dizziness, impaired vision, severe headaches (a sign of dehydration or elevated blood pressure), and decreased urine production. Midwives should clarify that these are not merely “fasting discomforts” but rather indicators that the body is having difficulty keeping its physiological equilibrium. Giving the mother a documented “Safety Checklist” gives her the confidence to know when her spiritual objectives must yield to medical necessity. To guarantee continuity of care, the midwifery team must record these educational sessions.
Nutritional Counseling: The “Nutrient-Dense” Window
The quality of the food a pregnant lady consumes between Iftar (sunset) and Suhoor (dawn) is crucial. She only has a short window of opportunity to eat the 2,500-2,700 calories needed for a successful pregnancy. As nutritional advisors, midwives should advise moms to avoid the deep-fried, high-sugar dishes that are frequently provided during Iftar parties since they contain “empty calories” and cause energy slumps.
Protein and hydration should be the main topics of the midwife’s advise. The growth of the baby’s brain and organs depends on protein. Greek yogurt, beans, eggs, and lean meats should be promoted to mothers. During the night, the midwife should recommend “Water-Loading” consuming two to three liters of water in numerous, little sips to stay hydrated. Another important piece of advice is to stay away from high-sodium dishes at Suhoor because too much salt would increase the mother’s thirst during the long daytime hours. The midwife helps the mother stay energized and gives the baby the building blocks it needs to grow by making the most of the non-fasting window.
Supporting the Decision: Cultural and Spiritual Sensitivity
The mother’s emotional support is arguably the most crucial component of midwifery guidance. It can be very emotional to decide whether or not to fast when pregnant. Some women experience pressure from family members, while others feel like a “failure” if they are unable to fast. A midwife who practices culturally sensitive care is aware that the decision is impacted by faith, culture, and identity in addition to medical facts.
Midwives should speak in a way that is encouraging and acknowledges the mother’s difficulties. It might be quite comforting to remind the mother that Islamic law prioritizes the health of the mother and child. If a woman chooses not to fast, the midwife might assist her in finding other ways to commemorate the month, including concentrating on charity or making additional prayers. If she fasts, the midwife becomes her “clinical partner,” kindly keeping an eye on her progress. This trusting relationship guarantees that the mother will feel comfortable seeking assistance from the midwife in the event of a problem without worrying about being condemned for her decision.
People Also Ask (FAQ)
Q: Does fasting during pregnancy cause low birth weight?
There is conflicting research on this. While some studies find no difference, others indicate that fasting during the second or third trimester may slightly raise the chance of low birth weight. Midwives use scans and fundal height to track fetal growth and make sure the infant is reaching its developmental goals.
Q: Can a pregnant woman take her prenatal vitamins while fasting?
Indeed! During the non-fasting hours, midwives strongly advise taking prenatal vitamins, particularly iron and folic acid. To maximize absorption and prevent upset stomachs, it is advisable to take them after a meal during Iftar or Suhoor.
Q: What is the most common reason a midwife tells a pregnant woman to stop fasting?
The most common clinical concern is dehydration. There may be less amniotic fluid surrounding the baby if the mother’s fluid levels are very low, as indicated by symptoms like dark urine, fainting, or excruciating headaches.
Q: Is it safe to fast in the first trimester if I have morning sickness?
If you are having frequent vomiting, midwives typically advise avoiding fasting. Rapid electrolyte loss and dehydration brought on by nausea and vomiting can be harmful to the mother and the developing embryo.
Q: How can I tell if I am dehydrated while fasting?
Take a look at the color of your pee. You are dehydrated if it is amber or dark yellow. Additional symptoms include an extremely dry mouth, dizziness when standing, and a rapid heartbeat. The midwife advises breaking the fast with water right away if you encounter these.
Useful Documents for every Nursing Student
CV Section Template for Nursing students
AHPRA – NMBA Registration Document Checklist (International Students-Graduates)
Clinical Placement Reflection Template (NMBA-aligned)
Cover Letter Template for Nursing Students
Disclaimer: “I researched this information on the internet; please use it as a guide and also reach out to a professional for assistance and advice.This information is not medical advice, so seek your medical professional’s assistance.”

