Summary
It is the hallmark of a nurse’s job, but in times of conflict and humanitarian need, it must be combined with extraordinary fortitude and specific clinical expertise. The healthcare infrastructure hospitals, clinics, and supply chains is frequently the first to suffer when a conflict arises. The transfer from a stable hospital to a conflict zone necessitates a drastic change in the way patient care is provided for nursing students and professional healthcare professionals. You are no longer only keeping an eye on a patient; instead, you are handling a situation in which essential supplies like antibiotics and painkillers, as well as electricity and clean water, might not be available.
Nurses become essential to survival in these high-stress situations. In addition to treating physical injuries, supporting patients during a conflict also entails managing psychological trauma, resolving difficult moral conundrums, and shielding the most vulnerable groups such as children and the elderly from the aftereffects of dislocation. This thorough guide offers nurses a useful road map for delivering excellent, life-saving care in the most difficult circumstances.
Triage and Mass Casualty Management in Conflict Zones
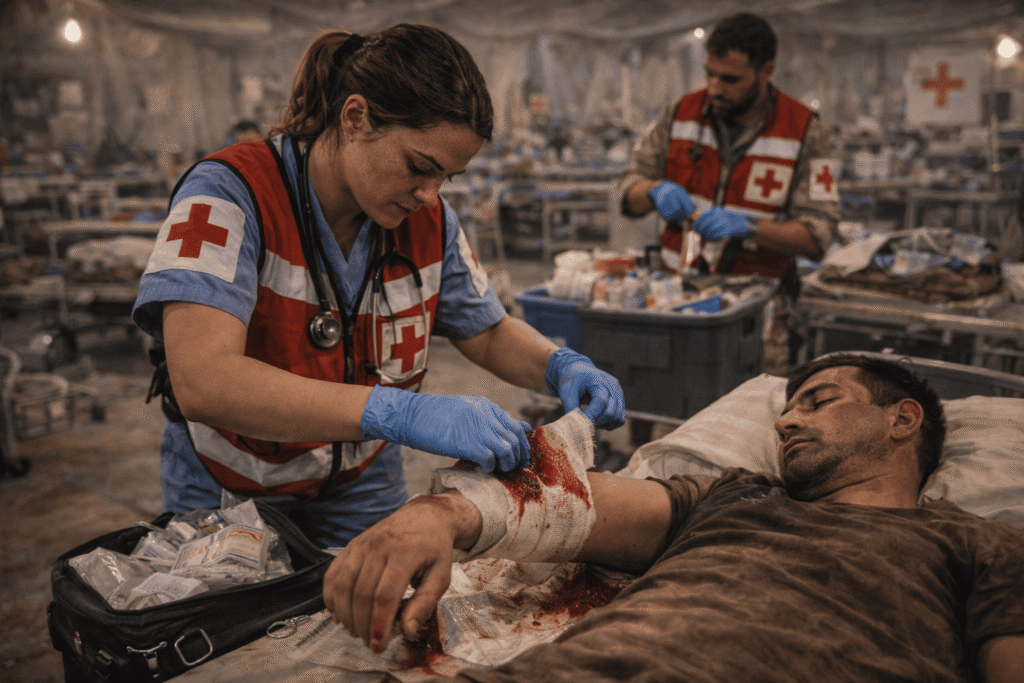
There are nearly always more injured patients than there are nurses and doctors accessible in a humanitarian crisis or an active combat zone. The most crucial skill in a nurse’s toolbox at this point is mass casualty triage. In contrast to a typical ER, when the “sickest” patient is seen first, wartime triage is predicated on “the greatest good for the greatest number.” Nurses must be able to swiftly classify patients according to their chances of survival and the resources needed to save them.
The START (Simple Triage and Rapid Treatment) approach is commonly employed by nurses. Patients are color-coded as follows: Green for “walking wounded,” Yellow for those who require care but can wait, Red for life-threatening conditions that can be treated right away, and Black for those who have passed away or have injuries so serious that they cannot be rescued with the resources available. Since it can be necessary to let one person go in order to save five others, this process is extremely draining. Effective triage, however, keeps the hospital from overcrowding and guarantees that few resources, like oxygen or blood bags, are used where they will have the biggest impact.
Tactical Clinical Care: Managing Trauma and Blast Injuries
Treating injuries that are uncommon in civilian life, such as blast trauma, landmine injuries, and high-velocity bullet wounds, is part of wartime nursing. Because blast injuries impact several organ systems simultaneously, they are especially complicated. The four stages of bomb injury—primary (pressure wave damaging lungs/ears), secondary (flying debris/shrapnel), tertiary (being flung by the blast), and quaternary (burns or chemical inhalation)—must be understood by a nurse.
Hemorrhage control is the main objective of tactical treatment. The most common avoidable cause of death in combat is uncontrolled bleeding. Nurses need to be proficient at applying tourniquets quickly and packing wounds with hemostatic gauze. Infection management is also quite difficult. Wounds are frequently infected with dirt and debris during a crisis. Nurses must prioritize vigorous wound cleansing and the prudent use of any available antibiotics in the absence of sterile operating rooms. Nurses serve as the first line of defense against the physical destruction of war by developing these trauma skills.
Psychological First Aid: Supporting Mental Health and Trauma
Even if they are not physically injured, every patient in a conflict zone suffers from trauma. Acute Stress Disorder and long-term PTSD are caused by the continuous sound of shelling, the death of family members, and the devastation of dwellings. The only persons a patient feels comfortable talking to are frequently nurses. Just as crucial as changing a bandage is administering Psychological First Aid (PFA). PFA is a useful strategy to lessen distress and help with urgent needs; it is not professional counseling.
For nurses in emergency situations, the “Look, Listen, Link” approach is the gold standard. Seek out people who are acting strangely or in shock; listen to their experiences without pressuring them to speak while maintaining a composed demeanor; and connect them to their loved ones or basic necessities like food and shelter. The trauma is especially severe for kids. at order to assist children understand the commotion around them, nurses might create “Safe Spaces” at the clinic where they can play or sketch. Nurses assist patients in starting the lengthy process of emotional healing by attending to the “invisible wounds” of war.
Continuity of Care for Chronic Conditions and Vulnerable Groups

The “Silent Killers” are chronic illnesses, but trauma takes center stage during a conflict. Patients with diabetes, hypertension, or kidney disease lose access to life-saving drugs and therapies when a city is under siege. Managing the “Continuity of Care” for these groups is part of a nurse’s job during a humanitarian disaster. Without insulin, a patient with diabetes may go into a coma; without blood pressure medication, a patient may have a stroke during a fight.
When handling these circumstances, nurses need to be creative. When a patient’s particular medication is out of stock, this may entail teaching them how to safely “ration” their medication or assisting them in finding alternate dietary strategies to control their blood sugar. Additionally, nurses have a duty to safeguard vulnerable populations, including elderly people and pregnant women. In bomb shelters or refugee camps, where women are compelled to give birth in filthy conditions, midwifery skills are frequently required. One of the main goals of humanitarian nursing is to make sure that these “forgotten” patients receive care.
Ethical Nursing and Professional Safety Under Fire
There are many ethical difficulties while working as a nurse in an armed situation. You might be required to treat a patient who is viewed as a “enemy,” or you might have to choose which youngster receives the final dose of an antibiotic that could save their life. Regardless of nationality, creed, or political affiliation, treatment must be given only on the basis of need, according to the International Code of Ethics for Nurses. Sustaining this “Medical Neutrality” is crucial for both the community’s trust and the healthcare team’s safety.
Another important factor is personal safety. Although hospitals and medical personnel are shielded from attack under the Geneva Conventions, this is not always upheld in contemporary combat. “Situational Awareness” training is required for nurses, which includes understanding the safest routes to work, recognizing “Hardened Spaces” in the hospital (areas away from windows), and knowing when to leave. If you become a casualty yourself, you cannot save lives. As a witness to history, ethical nursing in times of conflict also include the obligation to record, when safe, any abuses of human rights or the use of illicit weapons against civilians.
People Also Ask (FAQ)
Q: Do nurses have to treat “enemy” soldiers in a war zone?
Indeed. Medical professionals are required by international humanitarian law and the nursing code of ethics to treat injured patients only on the basis of clinical necessity. Like any other patient, an injured “enemy” soldier must have their care prioritized based on the severity of their injury.
Q: What is the most important item in a nurse’s “Crisis Bag”?
Tourniquets and hemostatic gauze are the most crucial tools, aside from a stethoscope. The most common life-saving action a nurse will do during a dispute is to stop significant bleeding.
Q: How do nurses manage without electricity in a hospital?
The nurses go back to “Manual Skills.” This entails using “Flashlight Nursing” for nighttime procedures, manually checking pulses rather than using a monitor, and counting respirations. In order to keep patients alive, many hospitals in conflict areas also use manual ventilators (Ambu-bags) or solar-powered lamps.
Q: Can nursing students help in a humanitarian crisis?
Indeed. Although they should adhere to their “scope of practice,” students are essential for helping with triage, healing wounds, documenting patients, and offering psychological support. Volunteering with groups like the Red Cross or Red Crescent provides many students with priceless experience.
Q: What is “Moral Injury” in nursing?
The psychological suffering brought on by having to make choices that contradict your own beliefs, such deciding which patient to save when resources are scarce, is known as moral harm. It is highly prevalent in conflict areas, and nurses require strong peer support to deal with these emotions.
Useful Documents for every Nursing Student
CV Section Template for Nursing students
AHPRA – NMBA Registration Document Checklist (International Students-Graduates)
Clinical Placement Reflection Template (NMBA-aligned)
Cover Letter Template for Nursing Students
Disclaimer: “I researched this information on the internet; please use it as a guide and also reach out to a professional for assistance and advice.This information is not medical advice, so seek your medical professional’s assistance.”
